About the author: Matthew Bonn is a research assistant at Dalhousie University and is also program coordinator with the Canadian Association of People Who Use Drugs.
In 2018, there were 83,483 drug arrests in Canada. That amounts to approximately 228 drug arrests on any given day.
We’ve been hearing a lot about police enforcing health protection acts during the coronavirus pandemic. But what are they doing about personal drug use of controlled substances during the pandemic?
Authorities should be considering the decriminalization of drugs during COVID-19 and implementing safe supply programs. Drug users are already one of the most marginalized and stigmatized populations in society without a pandemic, and unless we decriminalize drug use, they will bear the brunt of another deadly disease.
Policy-makers are beginning to listen to recommendations from people who use drugs. There have been federal exemptions allowing pharmacists more flexibility in renewing, refilling and transferring prescriptions, including narcotics. This has paved the way for a more patient-centred approach for implementing a plan for safer supply.
B.C. leads the way
After years of advocacy for a safer pharmaceutical alternative to the supply of toxic illegal drugs, the pandemic prompted British Columbia to create guidelines encouraging doctors to prescribe hydromorphone, morphine, dexedrine, methylphenidate (Ritalin) and diazepam — all controlled substances — to patients with substance use disorders.
Provincial correctional facilities are also releasing prisoners into the community to try to reduce the spread of COVID-19, although it’s unclear what will happen to them once it’s contained.

These are big steps for people who use drugs, but there’s no comprehensive and sustainable federal plan to reduce overdose fatalities and COVID-19 infections among some of our most marginalized citizens. Nor are there any plans to stop criminalizing them during COVID-19.
As police enforce health protection acts in cities all over Canada, we haven’t heard specifically what they plan to do about possession of controlled substances charges for people who have to buy their drugs on the street in the midst of COVID-19.
Read more: Why some Canadian prisoners should be released during the coronavirus pandemic
Is the plan to release inmates from provincial jails without adequate housing or social support, which could lead to them either contracting COVID-19 on the streets or being arrested for illegal drug activity and sent right back to jail? If so, that makes little sense.
Police going into high-risk areas
Drug possession and trafficking charges are the bread and butter of many police forces. There are undoubtedly still drug enforcement teams with ongoing investigations that involve investigators going in and out of COVID-19 “high-risk areas,” as chief public health officer, Dr. Theresa Tam, has noted.
We have heard reports of police officers not abiding by the same public health protocols as the rest of society to enforce the Quarantine Act.
News of officers testing positive for COVID-19 means they could transmit the virus to the communities they’re criminalizing. By decriminalizing drugs, we’ll be able to prevent police from potentially spreading COVID-19 to vulnerable communities.
Regardless of how police forces regard them, drug service providers, also known as drug dealers, are acting as service providers during this pandemic, supporting thousands of drug users who have not been able to access a safer medical supply.
There have always been safe pharmaceutical alternatives for opioids. But there has never been a safe supply of opioids for drug users. If doctors aren’t currently willing to provide patients with a safe supply, then drug users should have the legal right to buy what they need.
It’s time to change the way we look at people who use drugs and engage in criminal behaviour. We must remember many of them have endured profound, often lifelong trauma, have lived in poverty for much of their lives and must now function in a society that discriminates towards people who use drugs or have been incarcerated.
Doctors who wish to prescribe addictive drugs to their patients are supported by the British Columbia government. But while some patients are taking advantage of the B.C. measures, others can’t find a prescriber.
This isn’t a sustainable model for British Columbia, let alone the rest of Canada. Yet until all drugs are legal and regulated, it’s the only model we have. Doctors need to step up and prescribe a safe supply of drugs to drug users, not just in British Columbia, but everywhere in Canada.
Drug users are stuck
Drug users are already stuck in an ongoing criminogenic society that our system has created and operated for so long.
As soon as people are branded “addicts” or “criminals” by the state, the stigma and discrimination that have disseminated throughout society have a significant impact on their mental health. When you add a pandemic to the life of someone who uses drugs, the risks associated with the drug use escalate quickly as people are forced into isolation but continue to use alone.
We are starting to see the spike in overdose deaths in Vancouver and Toronto due to the pandemic. The disruption of services for people who use drugs is acutely life-threatening.
That’s why harm reduction services, safe consumption sites, overdose prevention sites and in-patient withdrawal management services must stay open. We are seeing them shut down or operating at extremely reduced capacity, but these are essential life-saving services. They can provide care while practising all public health protocols.
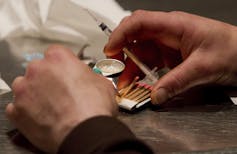
The prohibition of drugs has long created a huge demand for illicit drugs, leading to thousands of deaths and creating agony and heartbreak in our society. Many of us have lost a loved one due to this war on drugs.
Now is the time to decriminalize possession of drugs for personal use.
Every day, Prime Minister Justin Trudeau tells Canadians during his daily COVID-19 briefings that “nothing is off the table.” That should include decriminalization.
It may only be temporary, but it would provide a precedent to once and for all change Canada’s drug legislation. What we can accomplish now may last for a lifetime.![]()
This article was first published on The Conversation,
which features includes relevant and informed articles written by
researchers and academics in their areas of expertise and edited by
experienced journalists.
Dalhousie University is a founding
partner of The Conversation Canada, an online media outlet providing
independent, high-quality explanatory journalism. Originally established
in Australia in 2011, it has had more than 85 commissioning editors and
30,000-plus academics register as contributors. A full list of articles
written by Dalhousie academics can be found on the Conversation Canada website.

